Heart Block
What is heart block?
Electrical signals control the beating of your heart. They tell your heart muscle when to contract, a process known as conduction. The normal timing of heartbeats is generated in the upper chamber of the heart (atria) in a structure called the sinus node. The signal moves from the sinus node through the atria, causing contraction in the upper chambers. It then passes to the lower chambers (ventricles) of the heart, causing a contraction in the ventricles. When you have heart block, there is interference with the electrical signals that usually travel from the atria to the ventricles. This is known as a conduction disorder. If the electrical signals can’t move from your atria to your ventricles, they can’t tell your ventricles to contract and pump blood correctly.
Heart block is categorized as first-, second-, or third-degree:
- First-degree heart block. This is the least severe and most common type of heart block. The electrical signals are not completely blocked but slow down as they move from your atria to your ventricles. They continue to reach the ventricles without interruption, just slower than normal. You generally don't need any treatment for first-degree heart block.
-
Second-degree heart block. This means
that the electrical signals between your atria and ventricles can intermittently fail
to conduct. There are 2 types of second-degree heart block:
- Mobitz type I. (Also known as Wenckebach block.) The electrical signals get slower and slower between beats. Over time your heart drops a beat and then the process repeats. This is a less severe form of heart block and may not need immediate treatment.
- Mobitz type II. The electrical signals sometimes get to the ventricles, and sometimes they don't. There is no progressive slowing of the electrical signal. This type of heart block can often progress to third-degree heart block and is, therefore, more dangerous.
- Third-degree heart block (complete heart block). This is the most severe. In this type of block, electrical signals don't pass from your atria to your ventricles at all for periods of time. There is a complete failure of electrical conduction. This can result in no pulse or a very slow pulse if a backup heart rate within the ventricles are present.
What causes heart block?
If you are born with heart block, it's called congenital heart block. It's caused by a condition your mother had during her pregnancy or heart problems you were born with.
For most people, heart block develops as you get older. It happens when the electrical signals that connect the top and bottom of the heart develop fibrosis and eventually fail. Sometimes this may happen because of advancing age. Any process that can damage these electrical signals can result in heart block. Coronary artery disease with and without a heart attack is 1 of the most common causes of heart block. Diseases that weaken the heart muscle (cardiomyopathies) can also damage the electrical signals. Heart block can also be caused by any disease that can affect the heart, such as sarcoidosis and certain cancers, or any disease that results in heart inflammation. This can be an autoimmune disease or infection. Electrolyte problems, such as high potassium levels, can also result in heart block. Additionally, some heart surgeries can damage the conduction pathway leading to heart block. Certain heart medicines can also cause varying degrees of heart block.
Who is at risk for heart block?
You may be born with heart block (congenital). But many cases of heart block occur because of some other condition or event. These include:
- Older age
- Heart attack or coronary artery disease
- Cardiomyopathy
- Sarcoidosis
- Lyme disease
- High potassium levels
- Advanced kidney disease
- Severe hypothyroidism
- Certain inherited neuromuscular diseases
- Medicines that slow the heart rate
- After heart surgery
What are the symptoms of heart block?
Symptoms depend on the type of heart block you have: First-degree heart block may have no symptoms.
Second-degree heart block might cause:
- Dizziness
- Fainting
- The feeling that your heart pauses for a beat
- Trouble breathing or shortness of breath
- Nausea
- Severe tiredness (fatigue)
Third-degree heart block can be fatal. In addition to the symptoms above, it might cause:
- Intense tiredness
- Lightheadedness or fainting
- Irregular heartbeats
- Cardiac arrest
How is heart block diagnosed?
To diagnose your condition, your healthcare provider will consider:
- Your overall health and health history
- Any family history of heart block or heart disease
- Medicines you are taking
- Lifestyle choices, such as smoking or using illegal drugs
- Your description of symptoms
- A physical exam
- An electrocardiogram (ECG) that records your heart’s electrical impulses
- Testing with a Holter or event monitor to track your heart’s rhythm for a period of time. You might wear a Holter monitor for 24 or 48 hours, or even up to several weeks with some models. An event monitor can be worn for a month or more. These help capture changes in your heart’s rhythm, even if they don't occur often or predictably.
- Implantable loop recorder. This is a small heart recorder that is placed under the skin over the heart. It can record up to 3 years and is useful in cases where irregularities in conduction occur very rarely.
- An electrophysiology study. This is an outpatient procedure in which thin, flexible wires are threaded from your groin or arm to your heart to test the heart's electrical activity.
How is heart block treated?
You treatment depends on the type of heart block you have:
- Changes may be made in your medicines, or related underlying conditions may be treated.
- With first-degree heart block, you might not need treatment.
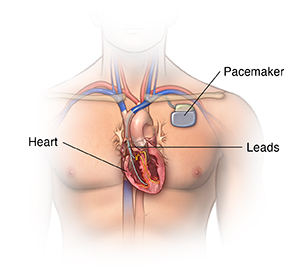
- With second-degree heart block, you may need a pacemaker if symptoms are present or if Mobitz II heart block is seen.
- With third-degree heart block, you will most likely need a pacemaker.
What are possible complications of heart block?
Complications of heart block may include fainting with injury, low blood pressure, damage to other internal organs, and cardiac arrest.
Can heart block be prevented?
Pregnant women who have an autoimmune disease may be able to get certain treatment to reduce the risk for heart block in their babies.
Prevention of heart block focuses mainly on managing the risk factors. A healthy lifestyle helps overall good health, including heart health. Exercise, eat a well-balanced diet, and don’t smoke. Understanding the risks of your medicines and reviewing them with your healthcare provider can reduce the risk for medicine-induced heart block. Talk with your healthcare team before taking any herbal supplements or new medicines, especially if you have risk factors for heart block.
Living with heart block
Follow your healthcare provider’s advice for taking medicine and using a pacemaker, if that applies to you. Also always keep follow-up appointments to make sure your treatment is on track.
To improve your quality of life with a pacemaker, you may need to:
- Stay out of situations in which your pacemaker may be disrupted. This includes not being near any electrical devices with strong magnetic fields.
- Carry a card that lets people know what kind of pacemaker you have.
- Tell all of your healthcare providers that you have a pacemaker.
- Get routine pacemaker checks to make sure your device is working well.
- Stay active, but don't take part in contact sports.
- Wear a medical alert bracelet or necklace.
When should I call my healthcare provider?
Get medical care right away for these symptoms:
- Severe tiredness
- Dizziness
Call 911
If you have sudden cardiac arrest, you won't be able to get care for yourself. It's very important to make sure the people you see on a regular basis know what to do in an emergency. Calling 911 is the most important first step. Also call 911 right away for these symptoms:
- Shortness of breath
- Chest pain
- Fainting or loss of consciousness
Key points about heart block
- Heart block occurs when the electrical signals from the top chambers of your heart don’t conduct correctly to the bottom chambers of your heart.
- There are 3 types of heart block. First-degree heart block may cause few problems. Third-degree heart block can be life-threatening.
- Heart block may cause no symptoms. Or it may cause dizziness, fainting, the feeling of skipped or irregular heartbeats, trouble breathing, fatigue, or even cardiac arrest.
- Depending on your degree of heart block, you may not need treatment. For some, a pacemaker is advised.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
- Know the reason for your visit and what you want to happen.
- Before your visit, write down questions you want answered.
- Bring someone with you to help you ask questions and remember what your provider tells you.
- At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
- Know why a new medicine or treatment is prescribed, and how it will help you. Also know what the side effects are.
- Ask if your condition can be treated in other ways.
- Know why a test or procedure is recommended and what the results could mean.
- Know what to expect if you do not take the medicine or have the test or procedure.
- If you have a follow-up appointment, write down the date, time, and purpose for that visit.
- Know how you can contact your healthcare provider if you have questions.
Connect with providers for illnesses like flus, UTIs and rashes (ages 3+) or chronic conditions like asthma, weight management and diabetes (ages 18+).
Cedars-Sinai has a range of comprehensive treatment options.

