Right Bundle Branch Block
What is right bundle branch block?
Right bundle branch block can affect the heart's rhythm.
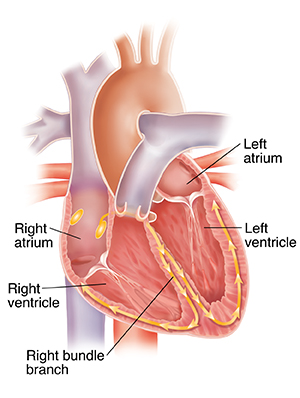
Your heart has 4 chambers. The top two chambers are called atria. The bottom two chambers are called ventricles. In a healthy heart, the electrical signal for your heartbeat starts in the sinoatrial (SA) node. The SA node is in the right atrium. The signal spreads from the SA node throughout the atria (upper chambers). Then the signal travels through the atrioventricular (AV) node to special fibers called the His bundle and bundle branches. These fibers spread the signal to the ventricles (lower chambers). As the signal moves, it helps the heart muscle contract in a smooth way. This is your heartbeat.
Two of the special groups of fibers are called the left and right bundle branches. They carry the signal from just below the AV node (where the top and bottom chambers of the heart meet) through the ventricles (bottom of the heart).
In right bundle branch block, there's a problem with the right branch, which sends the signal to the right ventricle. The signal can’t travel down this path the way it normally would. It still gets to the right ventricle, but it has to travel to the left side before getting there. This takes more time. Because of this, the right ventricle contracts a little later than it normally would. This can cause the heart to pump slightly less blood.
Some people with right bundle branch block don't have any symptoms unless they have some other heart condition.
Right bundle branch block is rare in healthy young people. It happens more often in older people. This may be due to the normal changes in the heart that occur with age. It can also happen in people who have another heart or lung problem. Or it may happen due to a heart procedure.
What causes right bundle branch block?
Right bundle branch block can result from conditions such as:
- Heart disease from high blood pressure in the lungs (pulmonary hypertension).
- Chronic obstructive lung disease (COPD).
- Blood clot in the lung (pulmonary embolism).
- Right-sided heart failure (cor pulmonale).
- Disease of the heart muscle (cardiomyopathy).
- Inflammation of a membrane surrounding the heart (myocarditis).
- Heart attack.
- Heart disease that exists from birth.
- Inherited arrhythmia syndromes (pseudo right bundle branch block).
- Medical procedures done on the heart.
Sometimes right bundle branch block occurs on its own, even when the heart's structure is normal. In these cases, experts aren’t sure what causes it. But typically it's not something to be concerned about.
Right bundle branch block sometimes happens after certain procedures. For example, it might occur for a while when a right heart catheter is inserted.
What are the symptoms of right bundle branch block?
Usually, right bundle branch block by itself doesn't cause symptoms. It's rare, but it may make symptoms worse in some people who have heart failure. Symptoms are more likely if you have other problems along with it.
How is right bundle branch block diagnosed?
Your doctor may use an electrocardiogram (ECG) to diagnose the problem. This checks your heart's electrical system. It can detect right bundle branch block. People often find out they have it when they have an ECG done for some other reason.
Your doctor might want to check you for other medical problems. You may get a complete medical history and physical exam. Along with the ECG, you might have these tests:
- Echocardiogram. This examines blood flow in the heart and heart motion.
- Lung tests.
- Blood tests.
How is right bundle branch block treated?
In healthy people who don't appear to have heart disease, right bundle branch block doesn't seem to have much effect on how long they live. They may not need any treatment at all for it. But they need to be checked closely after they are diagnosed.
In people with known or suspected heart disease, there's a greater risk of death. This is especially true after a heart attack.
Some people with right bundle branch block may someday need a permanent pacemaker. But this is rare. It's usually needed only when there's another heart electrical problem along with right bundle branch block.
How do you manage right bundle branch block?
You may get instructions about how to manage your right bundle branch block and overall heart health. You might need to make lifestyle changes. These may include:
- Losing weight.
- Quitting smoking.
- Eating a healthier diet.
You'll likely also need to:
- Watch your symptoms closely. Make sure you see a doctor on a regular basis, even if you don’t have any symptoms.
- Make sure all your doctors know about your right bundle branch block.
When should you contact your doctor?
Call 911 right away if you have severe symptoms like chest pain, fainting, or severe shortness of breath. If you have any new symptoms, see your doctor as soon as possible.
Key points about right bundle branch block
- Right bundle branch block affects the heart’s electrical conducting system. The right branch of this system is blocked or partly blocked. This makes the right ventricle contract a little later than it should.
- Follow your doctor's instructions closely. Take all your medicines as prescribed.
- If you have this condition, see your doctor for follow-up visits, as advised. Do this even if you don’t have any symptoms.
- You may need treatment for other health conditions.
- Most people with right bundle branch block may not need treatment. But some people may eventually need a pacemaker.
- Tell your doctor if you have severe symptoms or if they get worse.
Next steps
Here are some tips to help you get the most from a visit to your doctor:
- Know the reason for your visit and what you want to happen.
- Before your visit, write down questions you want answered.
- Bring someone with you to help you ask questions and remember what your doctor tells you.
- At the visit, write down the name of a new diagnosis. Note any new medicines, treatments, or tests. Also write down any new instructions your doctor gives you.
- Know why you're getting a new medicine or treatment and how it will help you. Also know what the side effects are.
- Ask if your condition can be treated in other ways.
- Know why a test or procedure is advised and what the results could mean.
- Know what to expect if you don't take the medicine or have the test or procedure.
- If you have a follow-up visit, write down the date, time, and purpose for that visit.
- Know how you can contact your doctor if you have questions.
Connect with providers for illnesses like flus, UTIs and rashes (ages 3+) or chronic conditions like asthma, weight management and diabetes (ages 18+).
Cedars-Sinai has a range of comprehensive treatment options.

